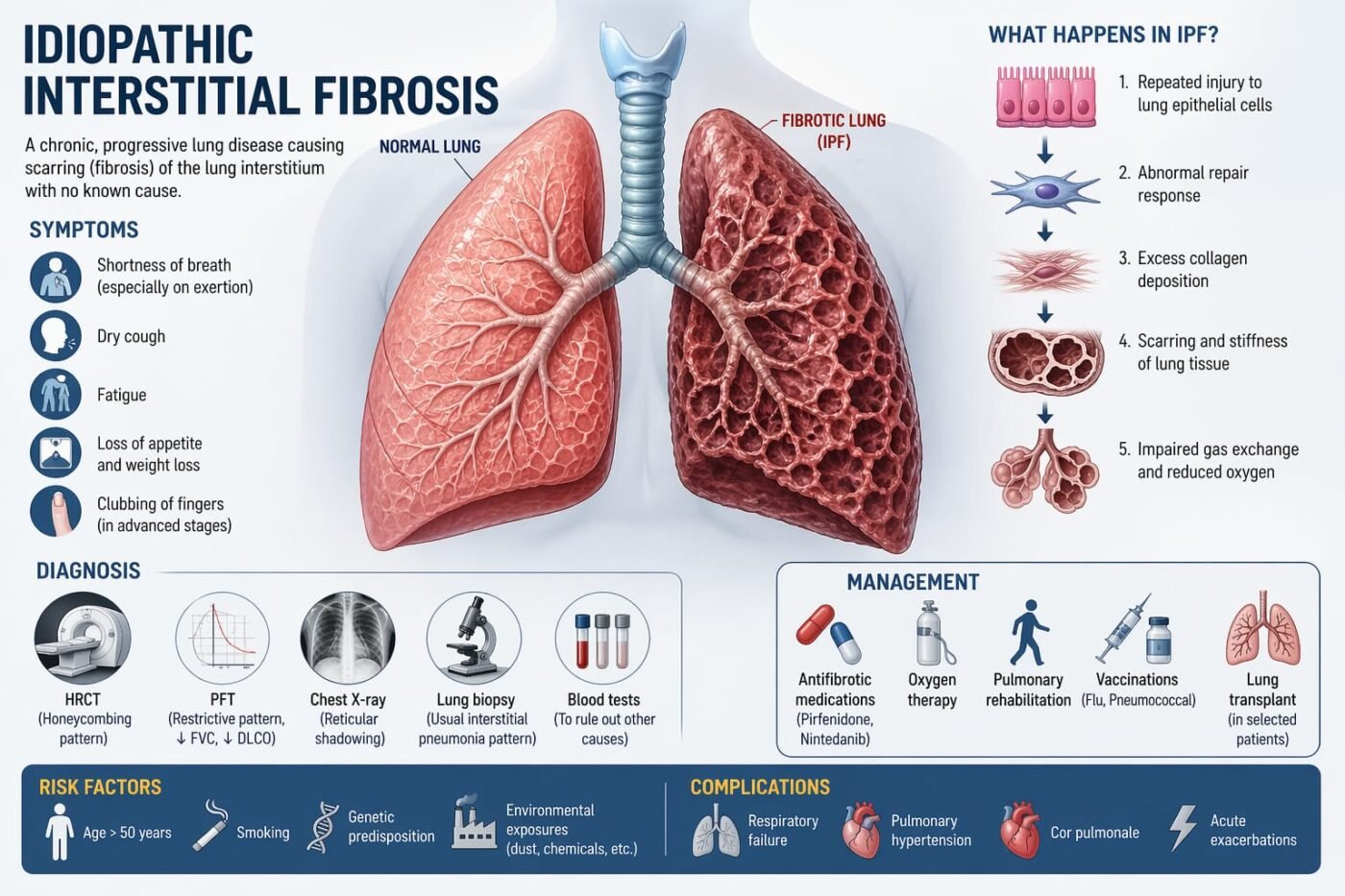
Idiopathic Pulmonary Fibrosis is a chronic, progressive lung disease that causes progressive scarring (fibrosis) of the lung tissue without a known cause. Over time, this scarring makes it increasingly difficult for the lungs to function properly, leading to persistent breathlessness and reduced oxygen supply to the body.
What is Idiopathic Pulmonary Fibrosis?
Idiopathic means “unknown cause,” and pulmonary fibrosis refers to thickening and scarring of the lung interstitium (the tissue around the air sacs). In IPF, this scarring is irreversible and tends to worsen over time. The lungs become stiff, making it harder for them to expand and transfer oxygen into the bloodstream.
Causes and Risk Factors
The exact cause of IPF is unknown, but several risk factors are associated with it:
- Age: Most common in people over 50
- Smoking history: Strongly linked to disease development
- Genetic predisposition: Family history increases risk
- Environmental exposure: Dust, metal, wood, and agricultural exposure
- Chronic micro-injuries to lung tissue
Despite these associations, IPF is classified as idiopathic because no single cause is confirmed.
Pathophysiology
Repeated injury to lung epithelial cells triggers an abnormal healing response:
- Lung injury occurs (cause unknown)
- Repair process becomes dysregulated
- Excess collagen is deposited
- Lung tissue becomes scarred and stiff
- Gas exchange capacity declines
This leads to progressive respiratory failure over time.
Signs and Symptoms of IPF
IPF usually develops slowly. Common symptoms include:
- Progressive shortness of breath (especially on exertion)
- Dry, persistent cough
- Fatigue and weakness
- Unexplained weight loss
- Clubbing of fingers (in advanced stages)
- Fine crackles on chest auscultation (“Velcro crackles”)
Diagnostic Investigations of IPF
Diagnosis of IPF is based on clinical, radiological, and sometimes histological findings:
1. High-Resolution CT (HRCT)
- Shows honeycombing pattern
- Reticular opacities in lower lung zones
2. Pulmonary Function Tests (PFTs)
- Restrictive pattern
- Reduced Forced Vital Capacity (FVC)
- Reduced Diffusion capacity (DLCO)
3. Chest X-ray
- May show reticular shadowing in advanced disease
4. Lung Biopsy (if needed)
- Confirms usual interstitial pneumonia (UIP) pattern
5. Blood Tests
- Used to rule out autoimmune causes
Management of IPF
There is no complete cure, but treatment focuses on slowing progression and improving quality of life.
1. Antifibrotic Therapy
These agents are prescribed if the vital capacity is between 50 to 80%. These drugs do not improve cough and Shortness of breath but slow down the disease progression. The most common drugs are
- Pirfenidone
- Nintedanib
If the further 10% decline in lung function is seen then the drugs are discontinued.
2. Oxygen Therapy
- In the patients with low blood oxygen saturation
3. Pulmonary Rehabilitation
- Breathing exercises
- Physical conditioning
4. Symptomatic Treatment
- Cough suppressants
- Treatment of infections
5. Lung Transplant
- Only curative option in selected patients
Prognosis of IPF
IPF is a progressive disease with variable outcomes. Some patients remain stable for years, while others experience rapid decline. Early diagnosis and antifibrotic therapy can significantly slow disease progression.
Complications of IPF
There are manifold severe complications of IPF that are
- Respiratory failure
- Pulmonary hypertension
- Right heart failure (cor pulmonale)
- Acute exacerbations (sudden worsening)
Prevention and Lifestyle Advice
While IPF cannot be fully prevented, patients can reduce disease progression by:
- Avoiding smoking
- Limiting exposure to dust and chemicals
- Staying physically active within tolerance
- Receiving vaccinations (influenza, pneumococcal)
Conclusion
Idiopathic Pulmonary Fibrosis is a serious lung condition characterized by progressive and irreversible lung scarring. Although its cause remains unknown, modern treatments and life style modification can slow its progression and improve quality of life. Early diagnosis and specialist care play a key role in managing this condition effectively.
Informative content 👌